American Pit Viper Snake Bites
Pit Vipers (sub-family Crotalinae) = rattlesnakes, cottonmouths (aka water moccasins), and copperheads
- See Pit Vipers of North Carolina for information on snake identification
Presentation :
- Classically presents w/ two puncture wounds, though a singular puncture wound does not exclude snake bite
- Some are "dry bites" (~25% of bites) with no venom injected and thus minimal symptoms

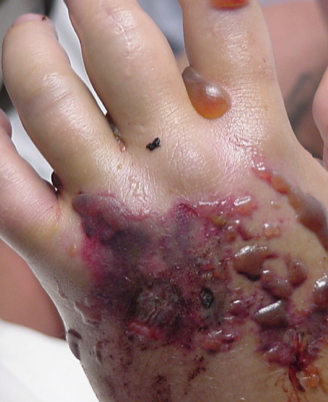
- Local toxicity: erythema, swelling, ecchymoses, pain (typically within 1h, up to 8+h). Tissue necrosis may develop.
- Bites to the fingers or toes may result in autoamputation
- Rattlesnake bites (particularly to upper extremities) can cause hemorrhagic bullae (40% of pts)
- Hematologic Toxicity: Prolonged PT/Inc INR, thrombocytopenia, and hypofibrinogenemia (akin to DIC). Nonetheless, frank bleeding/life-threatening bleeding is rare.
- Neurotoxicity: Uncommon; perioral/extremity paresthesias, bulbar abnormalities (eg, dysarthria, dysphagia), and myokymia (fasciculations of the face and proximal extremity muscles)
- Systemic:
- Severe Envenomation: Nausea, vomiting, diarrhea, tachycardia, paresthesias, hypotension, and dizziness
- Life-threatening Envenomation: Bleeding, hypotension, myokymia, weakness, and altered mental status
Pathophysiology :
- Venom contains a complex mixture of toxins, including phospholipase A2 (destroys membrane phospholipids), serine proteases (cleaves proteins), metalloproteinases (destroys extracellular matrix), thrombin-like enzymes (precipitating a DIC-like syndrome), etc
Diagnostic Testing:
- Signs/Symptoms may not develop immediately, monitor for 8-12h minimum up to 24h for high risk groups
- Draw a mark around the wound to monitor expansion, trend q15-30min
- CBC, PT/INR, fibrinogen to assess for hematologic toxicity; trend q6-8h
- BMP, CXR, EKG for systmic toxicity
- CK for compartment syndrome + neurotoxicity
- All patients who receive antivenom require follow-up monitoring (protocol based on product used) as late hemotoxicity may occur up to 14d later
- Monitor swollen extremities for compartment syndrome
Treatment :
- Consult with local poison control center
- First Aid:
- Remove any rings, watches, or constrictive clothing from the affected extremity.
- DO NOT apply pressure immobilization, tourniquets, or constrictive dressings as they worsen local tissue injury and there are no studies showing benefit in reducing systemic toxicity
- Oral suction of venom IS NOT recommended as it does not remove significant venom but increases risk of infection w/ oral flora
- First manage ABCs.
- Bites to face/neck are particularly high risk for progressing to airway obstruction and may merit intubation
- Myokymia that is extensive, or involves the muscles of respiration, is associated with respiratory failure
- Shock may develop requiring circulatory support
- Administer tetanus vaccine PRN
- Wound care: cleanse bite site with antiseptic (iodine or CHG), remove visible foreign bodies, elevate extremities to promote drainage of edema
- Prophylactic antibiotics for SSTI are not typically necessary, infection is rare unless wound is heavily contaminated
- Antivenom: should be given in consultation with poison control
- Typically indicated for:
- Bites to face/neck w/ swelling
- Significant local swelling w/ progression
- Hemotoxicity (elevated PT/INR, thrombocytopenia, hypofibrinogenemia)
- Does not improve with coagulation factor replacement
- Neurotoxicity
- Systemic toxicity: hypotension, bleeding distant from site of bite, refractory vomiting/diarrhea
- Administer in monitored setting (ER/ICU) to monitor for allergic reaction. Treat allergic rxn/Anaphylaxis as per usual
- Two approved antivenom products in US:
- CroFab: Ovine Crotalidae Polyvalent-immune Fab (FabAV)
- Contraindications: allergy to papain, papaya, or FabAV
- Requires maintenance doses to prevent recurrent toxicity (every 6 hours x3)
- Anavip: Equine Crotalidae Immune F(ab')2 (Fab2AV)
- Contraindications: allergy to horse protein, or FabAV
- CroFab: Ovine Crotalidae Polyvalent-immune Fab (FabAV)
- Redosing may be required if toxicity remains uncontrolled; may also be needed in cases of late hemotoxicity
- Typically indicated for:
Prognosis:
References:
Created on: Thursday 06-06-2024